
The Phases of the Menstrual Cycle
Jan 31, 2022Pop Quiz! Which of these statements is true?
A. The menstrual cycle refers to the number of days you bleed/are on your period
B. The menstrual cycle refers to the first day of bleeding through the day before you start bleeding again
If you chose B, you are correct! The menstrual cycle includes 4 phases - menstruation, follicular phase, ovulatory phase, and luteal phase. Bleeding days are part of the menstruation phase.
The 5th Vital Sign
The menstrual cycle can provide a lot of information about the overall health and wellness of a woman. In fact, the American College of Obstetricians & Gynecologists and the American Academy of Pediatrics have referred to the menstrual cycle as the fifth vital sign. Just like your pulse, temperature, respiration rate, and blood pressure, the menstrual cycle provides you with essential information about your health. Menstrual irregularities can indicate hormonal imbalances, gynecological diseases, or infections. Stress, changes in weight or diet, certain medications, and other lifestyle factors can cause temporary changes in the menstrual cycle.1
The Hormones of the Menstrual Cycle
To really understand the menstrual cycle, we also have to understand the main hormones involved in the menstrual cycle - follicle-stimulating hormone (FSH), luteinizing hormone (LH), estrogen, progesterone, and testosterone. Here are some key properties of each hormone.
Follicle-Stimulating Hormone (FSH)
- Essential for ovarian function
- Stimulates and matures the egg
Luteinizing Hormone (LH)
- Stimulates the release of the egg
- Stimulates the corpus luteum
Estrogen
- Creates the endometrium
- Regulates the menstrual cycle
- Plumps and moistens vaginal tissues
- Slows bone loss
- Reduces the incidence of heart attack
- Uplifts mood
- Increases libido
- Supports healthy cholesterol
- Positive effect on neurotransmitters
- Moisturizes skin
- Supports memory, reasoning, and fine motor skills
Progesterone
- Decreases menstrual bleeding
- Decreases fat storage
- Opposes estrogenic effects
- Improves brain function and memory
- Increases metabolic rate
- Required for conception and gestation
- Prevents PMS
- Anti-aging properties
- Supports mood and calms the nervous system
- Increases endurance
- Restores normal sleep patterns
Testosterone
- Improves mood
- Boosts libido
- Improves bone mineral density
- Increases muscles mass
Hormones are like a team sport where each one has a role to play and each hormone will affect the outcome of each cycle. The goal of each menstrual cycle is ovulation, even if conception is not your goal. However, ovulation can be the most difficult task of the menstrual cycle to achieve. While estrogen, progesterone, testosterone, FSH, and LH are the main stars of the menstrual cycle, they can also be impacted by other hormones. Cortisol, thyroid hormones, and insulin, in particular, can greatly influence sex hormones and ovulation. The endocrine system is a finely orchestrated system that works together on a negative feedback loop.
The Phases of the Menstrual Cycle
The menstrual cycle can be broken down into 4 phases -menstruation, follicular, ovulatory, and luteal. Throughout the 4 phases of your cycle, these hormones gently rise and fall at various times of your cycle. As I share more about the different phases, I'll base the information on a 28-day cycle. 28 days is the average length of the entire menstrual cycle encompassing these 4 phases. While 28 is average, anything between 25 and 35 days can be considered normal. What I want you to keep in mind and note is if you've had shifts away from what is NORMAL FOR YOU.
For example, let's say you have always been a 30-day cycle type of gal and suddenly your cycles are trending toward 26 days. Or you've been like clockwork every 27 days and suddenly you're consistently having 40-day cycles. You will want to investigate why your cycles have shifted. If your cycles tend to trend towards the 40-60+ length, that is something to explore with a qualified practitioner as well.
When referring to your menstrual cycle length, Day 1 is the very first day that you have menstrual flow. Spotting prior to the start of your period is not considered your period. The first day you have flow is considered day 1.
To calculate the actual overall length of your cycle start with Day 1 of menstrual flow all the way through the 4 phases until the day before you bleed again. This is your total cycle length.
So let’s dive into these phases a bit more and what’s actually happening to the hormones.
Menstruation - Days 1-6
Menstruation is characterized by the flow of dark/cranberry blood. FYI - Spotting is not considered the start of your period. We're talking actual flow here where you need to use a pad, tampon, cup, period panties, or menstrual disc.
Your period begins because implantation of a fertilized egg has not occurred and the corpus luteum has disintegrated. With that disintegration, progesterone and estrogen levels decline. The drop in hormones triggers the shed of the uterine lining.
The menstruation phase could actually be categorized as a sub-phase of the follicular phase. It's the rise in FSH and estrogen toward the end of your period that stops the menstrual flow. The average length to experience menstrual flow is 3-7 days.
Follicular - Days 7-13
Technically you enter the follicular phase when you begin menstruating. Menstruation is more like a subphase of the follicular phase. During the follicular phase, the pituitary gland sends follicle-stimulating hormone (FSH) to your ovaries to stimulate the eggs for maturation. While several eggs are stimulated and begin to mature, only one becomes the dominant egg for that cycle.
Estrogen is secreted by the egg that is dominant as it matures. This slowly increases overall estrogen levels. Rising estrogen levels begin to thicken the uterine lining in preparation for ovulation and implantation.
You’ll also begin to notice changes in your cervical mucus after menstruation. It may be absent at first and then become sticky or tacky.
Ovulatory - Days 14-21
Ovulation is the #1 goal of every menstrual cycle but it can be the hardest phase of the menstrual cycle to achieve. Ovulation is like the Super Bowl of the menstrual cycle. You need all of the team players (hormones) to be in sync and communicate well for ovulation to occur. This includes the sex hormones but can also be influenced by other hormones like cortisol, insulin, and thyroid hormones. (PLEASE NOTE, HORMONAL BIRTH CONTROL OF ANY KIND, INCLUDING HORMONAL IUDs, INHIBIT OVULATION)
The events that happen in the follicular phase are preparing the body for ovulation. The dominant follicle that is being stimulated by FSH in the follicular phase is secreting estrogen. A sharp rise in estrogen will switch off the FSH signal and switch on the luteinizing hormone (LH).
Estrogen levels fall dramatically immediately prior to the LH peak.2 A spike in LH occurs within 8-36 hours of the mature egg rupturing from the follicle - aka ovulation.
It’s important to note that this is the time that you are the most fertile. Knowing your ovulatory window is key if you are trying to conceive OR trying to avoid pregnancy. While an egg is viable for only 24 hours, sperm is viable for up to 5 days. Therefore, THERE IS A 6 DAY WINDOW IN WHICH YOU CAN BECOME PREGNANT. I write that with emphasis because I want you to really understand that you cannot get pregnant every single day of your cycle. If you have intercourse with a male up to 5 days prior and up to 24 hours after ovulation, you will need to know that conception is possible. Barrier methods of birth control are recommended to avoid pregnancy if that is not your goal.
Cervical fluid will also be a wet/slippery/egg-white-like substance. The change in viscosity creates a more hospitable environment for sperm to flow toward the egg. You can learn more about how to track your menstrual cycle here if you are trying to conceive or trying to avoid pregnancy.
The ovulatory phase of your cycle is also when you have a slight surge in testosterone. With that testosterone boost plus a surge of estrogen, you may notice that your libido improves as well during this phase.
Luteal - Days 22-28
Just like menstruation is a subphase of the follicular phase, you could say that ovulation is a subphase of the luteal phase. The luteal phase (including post-ovulation) of the cycle is relatively constant in all women, with a duration of 14 days.3
The corpus luteum (the sac left behind after ovulation) secretes progesterone and estrogen. These hormones will peak around day 21 and then slowly start to fall if implantation of a fertilized egg has not occurred. Implantation will usually occur within 8 days of fertilization. Progesterone should be the prevailing hormone during the luteal phase even after the corpus luteum disintegrates.
Cervical fluid will be sticky or absent during this phase as hormone levels fall. PMS symptoms may occur during this phase especially if there is a hormonal imbalance. *NOTE-Just because something is common, like PMS symptoms, does not necessarily mean it is normal. Testosterone can rise slightly towards the end of this phase as well.
It’s the fall of progesterone and estrogen that will trigger the shed of the uterine lining and start the menstrual cycle again.
Check out this image for an illustration of the rise and fall of hormones throughout the menstrual cycle.
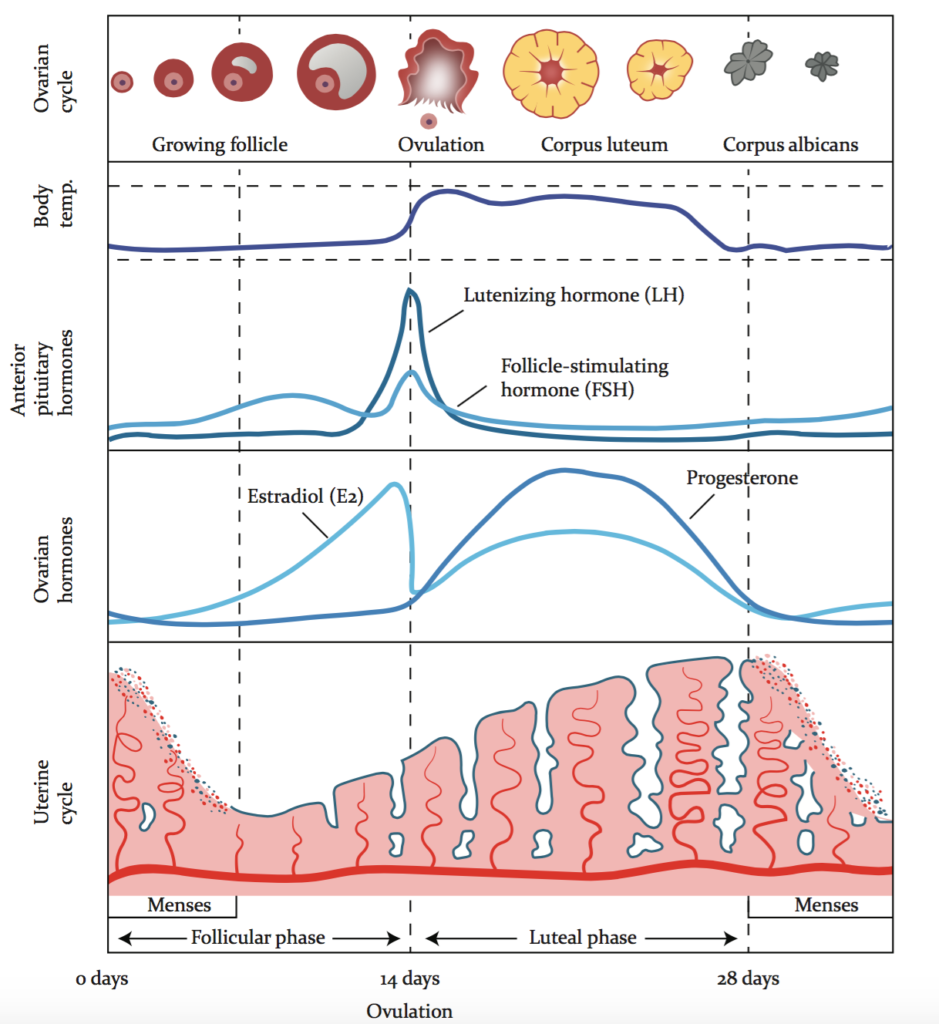
Image courtesy of Vios Fertility Institue
Testing Hormones
As you can see, the menstrual cycle is very complex with hormones changing every day! With that being said, I can’t emphasize enough that the day on which you test during your menstrual cycle is critical! For example, if you're interested in knowing your progesterone levels, you would want to check those between days 19-21 of your cycle (based on a 28-day cycle) while evaluating ovarian reserve should be evaluated between days 1-3.
There are a few different ways in which you can evaluate your hormones as well - blood (spot or serum), saliva, or urine. Below I have listed the advantages and disadvantages of each way to test hormones.
Blood Serum/Blood Spot
PROS:
- Easily defined reference ranges
- Can evaluate all hormones
- At-home testing for blood spot
CONS:
- In-office testing for blood serum
- Does not measure metabolites
Saliva
PROS:
- Easy to do multipoint measurements
- At-home collection
- Topical and oral hormones are well-represented
CONS:
- Does not measure metabolites
- Potential for false high reading
- Possible collection contamination
Urine
PROS:
- Wet or dried urine can be used to measure hormone metabolites
- Easy at-home testing
CONS:
- Wet urine results can be affected by kidney or liver issues
- Dried urine may not reflect hormone levels in the tissues if supplementing
Is this complex? Yes. Do you need to know all of this? No. But you do need to be in tune with your body and understand how your hormones are shifting. Use an app such as My Flo, Clue, or even your Apple or Garmin watch to track your symptoms. You can even just track them on the notes section on your phone. By doing this, a qualified practitioner can help to understand your symptoms and determine which testing or additional support you need.
Want to support your hormones nutritionally? Download my free Seed Cycling Guide to support the hormones of the menstrual cycle.

*The information available on this website is for general health information only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. You should not rely exclusively on information provided on the Website for your health needs. You can read more about our disclaimer here.*
References:
Are you overwhelmed by all of the conflicting information regarding health, hormones, nutrition, and weight management?
Join me once a month for a FREE "Ask Me Anything" live Zoom sesh! I'll answer all the questions you've been spending so much time searching the internet for.









